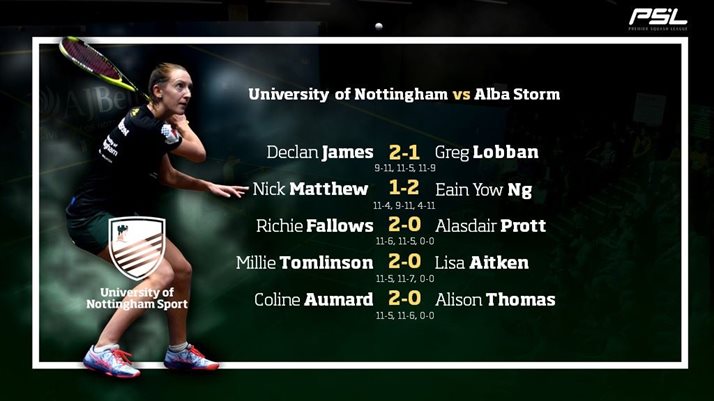
,, ,, That most of these studies fall in the range of moderate-to-good attests to the resilience of the NGS as a clinically useful grading system. The overall moderate interobserver agreement in this study applying the NGS (κ = 0.54) is similar to that described in other studies (κ = 0.43–0.83), including the largest study conducted in Nottingham which involved 600 raters (κ = 0.45). In addition, greater clinical weight should be placed on higher grades (3) assigned to CNB than the lower grades (1 < 2).įigure 1: A high-power fields exhibiting tumor cells with moderately pleomorphic nuclei and frequent mitotic figures (arrows) Based on these observations, greater clinical attention should be paid to adequate sampling, especially from tumor edges. Even though breast cancers are heterogeneous, mitosis is usually most active at the growing edges of tumors, and this can better be appreciated on surgical pathology when the entire tumor is excised than on CNB. In the index study, underscoring of mitotic count contributed significantly to underscoring of the overall grade, and this has been corroborated by other studies. No case was downgraded in our study compared to 7% reported by Zheng et al. ,, These differences may be due to fewer cores being submitted by our surgeons as well as interobserver variations based on pathologist's experience. while upgrading in 50% of our cases is higher than 24%–40% described by others. 
This was based on the observation that comparable grading was found when this technique was compared with microscopic grading.Ĭoncordance of 50% between CNB and surgical pathology in our study is lower than 69% documented by Zheng et al. Al-Janabi et al., on the other hand, have recommended whole-slide digital imaging as a panacea to the problem. 0.69 mm), having found this to be more reproducible. Bonert and Tate suggested standardization of the microscope field area and recommended the use of larger field areas (0.40 mm vs. Increasing the number of fields counted to between 20 and 30 was another suggestion, and they found to have correlated better with prognosis. Results: Kappa value (κ) for the first 43 cases was 0.50 (moderate agreement P 10 mitotic figures per ten 0.18 mm 2 hpf, having found this to better predict outcome in patients followed for 6.4 years. In the last 6 cases, consensus grades were assigned to both the initial core needle biopsy (CNB) and the excisional biopsy. The next 24 cases were graded independently by 4 pathologists and compared. These were grouped into 43 cases on which consensus grades assigned by 3 pathologists were compared with initial grades assigned to the cases. Materials and Methods: Slides of 73 cases of invasive carcinomas of the breast were retrieved from archives. Objective: The objective of this study is to audit interobserver agreement in grading and evaluate agreement of grading on core needle biopsies with surgical pathology. Thus, accurate and reproducible grading must be ensured by periodic auditing and training. Background: Histologic grade of breast cancer is a Category I prognostic factor.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
